“ExpiraFlow Technology represents a shift in the paradigm of ventilator COPD management toward more personalized therapy, which automatically optimizes ventilation to the individual needs of the patient,” said Peter Calverley, Professor of Respiratory Medicine, School of Aging and Chronic Disease at the University of Liverpool. “By monitoring the presence of EFL on a breath-by-breath basis, the A40 EFL system can automatically adjust therapy pressures to ensure efficient lung emptying and better gas exchange. This new focus allows us to consider individual differences in lung mechanics and gas exchange when managing complex respiratory patients,” says Peter Calverley
Chronic obstructive pulmonary disease (COPD) is a chronic inflammatory lung disease that causes obstructed airflow from the lungs. Symptoms include breathing difficulty, cough, mucus production and wheezing. It is typically caused by long-term exposure to irritating gases or particulate matter, most often from cigarette smoke. People with COPD are at increased risk of developing heart disease, lung cancer and a variety of other conditions.
Emphysema and chronic bronchitis are the two most common conditions that contribute to COPD. These two conditions usually occur together and can vary in severity among individuals with COPD.
Chronic bronchitis is inflammation of the lining of the bronchial tubes, which carry air to and from the air sacs (alveoli) of the lungs. It is characterized by daily cough and mucus production.
Emphysema is a condition in which the alveoli at the end of the smallest air passages (bronchioles) of the lungs are destroyed as a result of damaging exposure to cigarette smoke and other irritating gases and particulate matter.
 Although COPD is a progressive disease that gets worse over time, COPD is treatable. With proper management, most people with COPD can achieve good symptom control and quality of life, as well as reduced risk of other associated conditions.
Although COPD is a progressive disease that gets worse over time, COPD is treatable. With proper management, most people with COPD can achieve good symptom control and quality of life, as well as reduced risk of other associated conditions.
The global mechanical ventilators market size is expected to reach $3.6 billion by 2027 according to a new report. The market is projected to register a CAGR of 4.7% from 2022 to 2027. The unprecedented dawn of COVID-19 pandemic, increasing incidence of Chronic Obstructive Pulmonary Disease (COPD), rising incidence of respiratory emergencies, and technological innovation in respiratory care devices are the major factors driving the market growth.
Technological advancements such as rapid innovation in the field of Positive Airway Pressure (PAP) devices, portability and improvement in the battery life of transport and portable devices are the factors driving the growth of the market. The World Health Organization (WHO) estimates that, at present, approximately 90% of COPD-related deaths occur in low- and middle-income countries.
Therefore, the rise in prevalence of such diseases, introduction, and availability of portable, cost contained, and easy-to-use mechanical ventilators for the treatment of respiratory conditions is expected to drive the growth in the demand for mechanical ventilators worldwide.
Non-invasive ventilator therapy
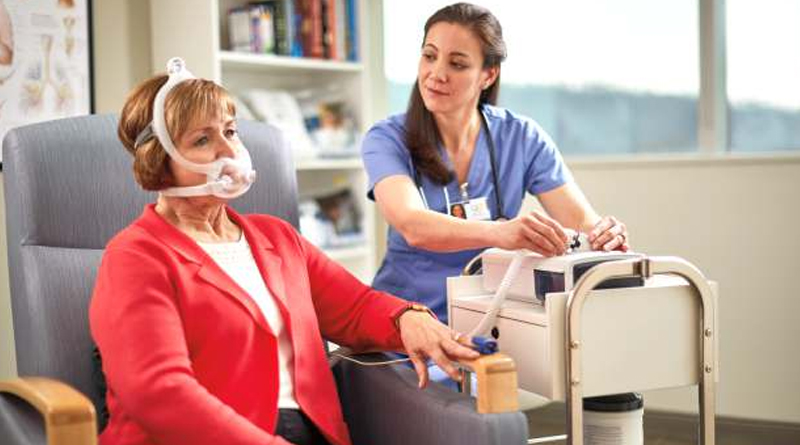
Royal Philips, a global leader in healthcare technology, recently announced the launch of Philips Ventilator BiPAP A40 EFL. With the introduction of this non-invasive ventilator, Philips extends its homecare solutions with a new ventilation therapy feature for chronic obstructive pulmonary disease (COPD) patients to breathe easier. Now, pulmonologists can identify COPD patients with expiratory flow limitation (EFL) and treat them with targeted therapy to reduce symptoms and increase their comfort while sleeping. The BiPAP A40 EFL ventilator continuously and optimally adjusts pressure based on patient needs.
BiPAP A40 EFL is the first and only non-invasive ventilator that allows health care professionals to automatically screen for and detect EFL, then provide optimal homecare therapy to dynamically and automatically abolish EFL [1]. This helps to reduce the patient’s work of breathing. Built with Philips proprietary and clinically validated ExpiraFlow technology, BiPAP A40 EFL is designed to connect across the care pathway – from diagnostic work to point of care therapy – to enable informed clinical decisions and optimize ventilation therapy, even remotely.
More than 50 percent of COPD patients experience EFL – limited exhalation of breath from the lungs – which occurs in the lower airways when patients are breathing quietly. EFL causes hyperinflation, or breathing at increased lung volumes. COPD patients with EFL are more likely to be hospitalized more often and have increased mortality rates, however EFL is difficult to detect and often undertreated, despite its prevalence. Philips unique ExpiraFlow technology automatically detects EFL more accurately than any alternate methods to enable the more effective treatment of patient in the home and help avoid hospital readmissions.
“ExpiraFlow Technology represents a shift in the paradigm of ventilator COPD management toward more personalized therapy, which automatically optimizes ventilation to the individual needs of the patient,” said Peter Calverley, Professor of Respiratory Medicine, School of Aging and Chronic Disease at the University of Liverpool. “By monitoring the presence of EFL on a breath-by-breath basis, the A40 EFL system can automatically adjust therapy pressures to ensure efficient lung emptying and better gas exchange. This new focus allows us to consider individual differences in lung mechanics and gas exchange when managing complex respiratory patients.”
 Revolutionizing COPD care solutions
Revolutionizing COPD care solutions
BiPAP A40 EFL aims to revolutionize COPD care solutions. Clinicians can now detect EFL in hypercapnic COPD patients at the point of care, ensure personalized patient treatment at home and monitor care remotely.
“EFL often goes undetected, meaning patients don’t receive the care they need to improve their disease,” said Eli Diacopoulos, Respiratory Care Business Leader at Philips. “At Philips, we’re committed to identifying these gaps and meeting the challenges that COPD patients face every day. BiPAP A40 EFL aims to revolutionize COPD care solutions. Clinicians can now detect EFL in hypercapnic COPD patients at the point of care, ensure personalized patient treatment at home and monitor care remotely.”
The BiPAP A40 EFL leverages Philips leading connected solution platform to streamline diagnostic work through integration to Philips Alice sleep lab and home diagnostic systems. When prescribed and used in the home, the BiPAP A40 EFL connects to Philips Care Orchestrator cloud-based care management system. By making it easier to analyze and share information, this connectivity enables providers to make faster, more informed clinical decisions, and identify and prioritize patients who are in need of therapy intervention to better manage chronic respiratory patient care from hospital to home.
BiPAP A40 EFL is CE marked and initially available in selected countries in Europe, with expansion in to additional European markets expected in 2021.